Warts Specialist

City Podiatry
Podiatrists located in Midtown, New York, NY
Warts can be unsightly and painful, and they may spread to other parts of your body or to other people if left untreated. Fortunately, there are many options for wart removal available at City Podiatry in New York City. If you have plantar warts or warts on the top of your feet, the board-certified podiatrists can help. Call the Midtown Manhattan office or schedule an evaluation online today.
Warts Q & A
What are warts?
Warts are growths caused by viral skin infections. They’re usually smaller than the head of a thumbtack, but they can sometimes grow larger.
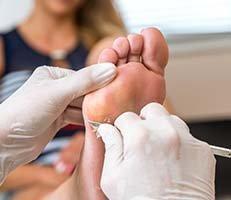
Plantar warts develop on the bottom of your feet or on your toes. Other types of warts can appear on the top of your feet as well.
Can warts be prevented?
Different types of warts are caused by different strains of the human papillomavirus (HPV), which can be spread to other people through skin-to-skin contact or by sharing an environment with someone who has a wart. Plantar warts are often transferred through shared shower facilities because the moisture in those environments helps keep the virus alive longer.
Follow these precautions to help prevent warts from spreading:
- Wash hands and feet frequently
- Don’t pick at warts
- Don’t touch your warts or someone else's
Even if you don’t have plantar warts, it’s a good idea to wear shower shoes in public pools, gyms, and other shared environments.
What are the symptoms of plantar warts?
You may have plantar warts if you have a small growth on the bottom of your foot with any of the following characteristics:
- Tiny dark spots
- Rough or spongy texture
- Scaly appearance
- Pain when walking or standing
If you’re unsure if your growth is a wart or not, it’s a good idea to have an evaluation by the team at City Podiatry to rule out any conditions that can lead to a severe complication.
Can I treat plantar warts at home?
Over-the-counter medications and freezing sprays are available, but these are much less effective than the treatments your doctor can provide. If you’ve tried over-the-counter treatment without success, it’s not advisable to repeat the treatment, as this can aggravate your discomfort.
You should never attempt to cut a wart off on your own. The caring podiatrists at City Podiatry can provide safe, effective treatments for your warts, many of which work quickly to alleviate your discomfort.
How does a podiatrist treat warts?
The experienced podiatrists at City Podiatry offer a range of options for treating warts. These include:
- Prescription-strength salicylic acid
- Canthacur, a more aggressive topical treatment
- Liquid nitrogen freezing
- Laser removal
- Surgical removal
- Swift® microwave therapy
The Swift system uses noninvasive microwave technology to destroy warts without needles or cutting. Laser treatments, as well as surgical options, are minimally invasive outpatient procedures. For more information, call City Podiatry or schedule an evaluation online today.
Click here to learn more about how Swift Microwave Therapy can get rid of your warts.
Conditions & Treatments
-
 Achilles Tendonitismore info
Achilles Tendonitismore info -
 Athlete's Footmore info
Athlete's Footmore info -
 Bunionsmore info
Bunionsmore info -
 Diabetic Foot Caremore info
Diabetic Foot Caremore info -
 Flat Feetmore info
Flat Feetmore info -
 Sprains and Strainsmore info
Sprains and Strainsmore info -
 Hammertoesmore info
Hammertoesmore info -
 Ankle & Foot Injuriesmore info
Ankle & Foot Injuriesmore info -
 Neuromasmore info
Neuromasmore info -
 Plantar Fasciitismore info
Plantar Fasciitismore info -
 Fungal Toenailsmore info
Fungal Toenailsmore info -
 Ingrown Toenailmore info
Ingrown Toenailmore info -
 Keryflexmore info
Keryflexmore info -
 Laser Nail Treatmentmore info
Laser Nail Treatmentmore info -
 Arthritismore info
Arthritismore info -
 Orthoticsmore info
Orthoticsmore info -
 PRP Therapymore info
PRP Therapymore info -
 Regenerative Medicinemore info
Regenerative Medicinemore info -
 Stress Fracturemore info
Stress Fracturemore info -
 Wartsmore info
Wartsmore info -
 Lapiplastymore info
Lapiplastymore info -
 Emergency Foot Caremore info
Emergency Foot Caremore info -
 Tenexmore info
Tenexmore info -
 Heel Painmore info
Heel Painmore info -
 Swift Microwave Therapymore info
Swift Microwave Therapymore info